Kalra Brain & Spine
At KBS, we treat our patients as neighbors, friends, and family. Our goal is to educate you, treat your symptoms, and help you recover as fast as possible
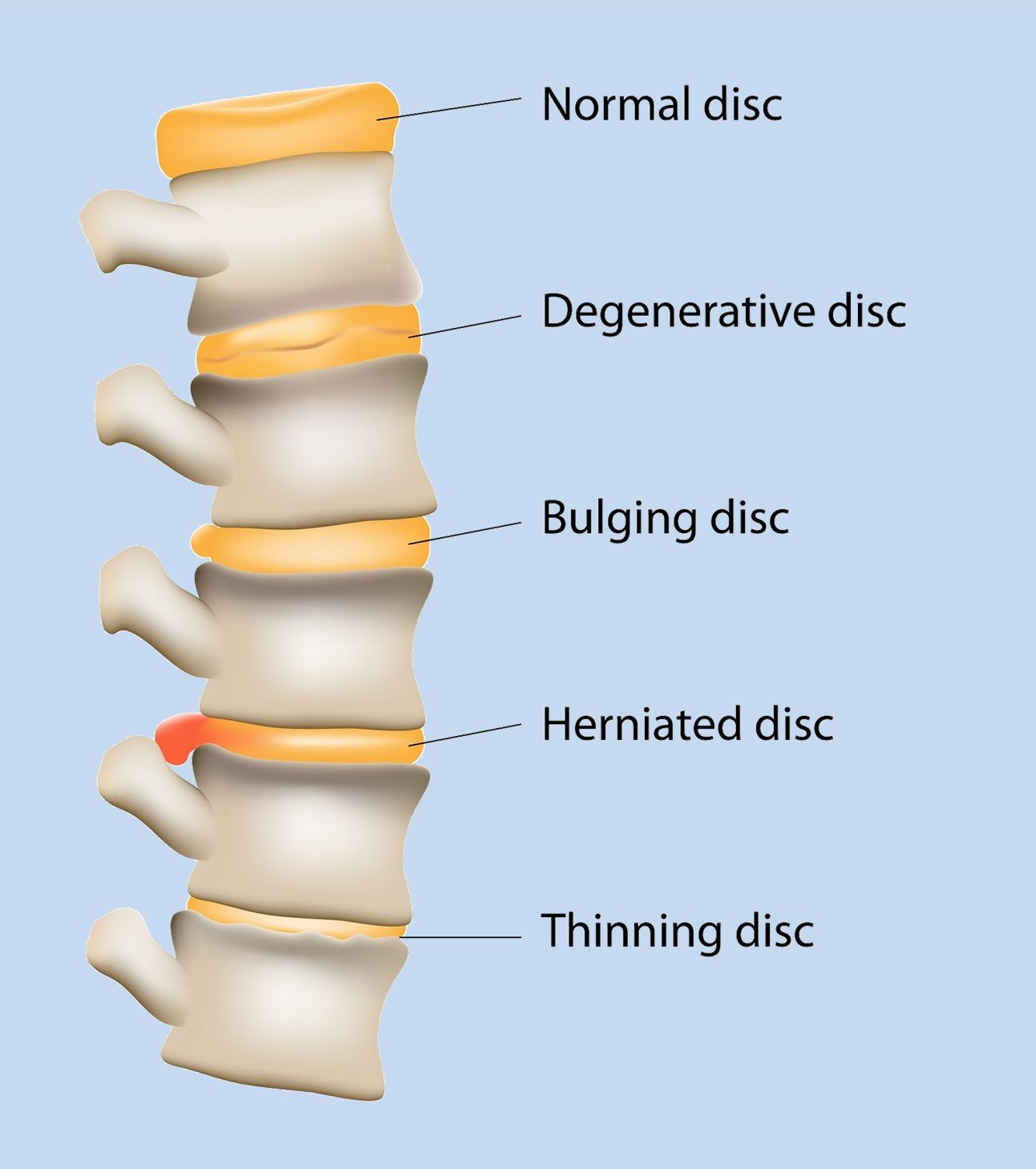
Degenerative Disc Disease
Nearly everyone’s spinal discs show signs of wear as they age. Not everyone, however, will have degenerative disc disease.
Not actually a disease, this is a condition in which a damaged disc causes pain. A wide range of symptoms and severity is associated with this condition.
The discs are like shock absorbers between the bones of the spine and are designed to help the back stay flexible while resisting terrific forces in many different planes of motion. Each disc has two parts:
- A firm, tough outer layer, the anulus fibrosus. The outer portion of this layer contains nerves. If the disc tears in this area, it can become quite painful.
- A soft, jellylike core, the nucleus pulposus. This part of the disc contains proteins that can cause the tissues they touch to become swollen and tender. If these proteins leak out to the nerves of the outer layer of the disc, they can cause a great deal of pain.
Unlike other tissues of the body, the disc has very low blood supply. Once a disc is injured, it cannot repair itself, and a spiral of degeneration can set in with three stages that appear to occur over 20 to 30 years:
- Acute pain makes normal movement of the back difficult
- The bone where the injury occurred becomes relatively unstable. Over a long period of time, the patient will have back pain that comes and goes.
- The body restabilizes the injured segment of the back. The patient experiences fewer bouts of back pain.
Symptoms
There may be no symptoms. But in some cases, the spine loses flexibility and bone spurs may pinch a nerve root, causing pain or weakness. If you have degenerative disc disease, you may experience:
- Pain in the legs, thighs, buttocks, lower back or neck
- Pins and needles or reduced sensation
- Muscle spasms
- Physical deformity and/or stiffness
- Nerve injury
Risk Factors/Causes
Several factors can cause discs to degenerate, including age. Specific factors include:
- The drying out of the disc. As we age, the disc dries out and doesn’t absorb shocks as well.
- Daily activities and sports can cause tears in the outer core of the disc
- Injuries can cause swelling, soreness and instability
Treatment Options
Getting back pain under control – no matter the source – requires exercise to increase the strength and flexibility of muscles that surround and support the spine. Exercising increases blood flow to the back, which nourishes joints and muscles with oxygen and nutrients, while clearing away destructive inflammatory waste products.
Treatment options to go along with physical activity and exercises to increase back strength include:
- Physical therapy
- Medications such as Tylenol and Ibuprofen
- Spinal injections
- Spinal fusion
- Heat and cold therapy
- Decompression surgery
- Disc replacement
New Hope From a Spine Expert
When world-class training meets hometown values deeply rooted in family and community, the result is the kind of medical care you’ve always hoped for. This describes Kalra Brain & Spine, the practice of Dr. Ricky Kalra, who specializes in the most up-to-date evidence-based neurological care. If your condition requires neurosurgery, schedule a consultation with Dr. Kalra today.
Request an Appointment
Contact us
Get In Touch
Address
Kalra Brain & Spine
5899 Preston Road
Suite 1303
Frisco, TX 75034
Phone
972-905-9226

Fax
972-905-9269